Options Multiply for 3D Printed Spinal Implants
June 21, 2018
Let’s hope you never need one, but if you do, a 3D printed spinal implant could be the key to pain relief for those with severe back problems. The source of that pain may be a damaged disc in the neck area (cervical), upper back (thoracic) or lower back (lumbar). Typical problems addressed are degenerative disc disease (DDD), degenerative scoliosis (abnormal sideways curvature) and degenerative spondylolisthesis (where one vertebra slips forward of the one below it).
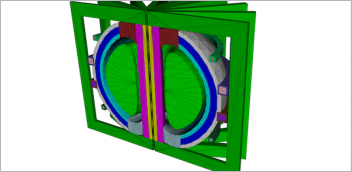
 3D printed titanium spinal implants from 4WEB Medical, showing the truss-and-strut-based open architecture that promotes bone in-growth while supporting optimal load bearing. (Image courtesy 4WEB Medical)
3D printed titanium spinal implants from 4WEB Medical, showing the truss-and-strut-based open architecture that promotes bone in-growth while supporting optimal load bearing. (Image courtesy 4WEB Medical)At a top level, the treatment involves first removing that disc from between two vertebrae. The surgeon then fills in the gap created by removal of the damaged disc with a spinal “cage” or implant, an often wedge-shaped piece with a purposely airy, open structure which allows bone to grow through it. Surgeons then use “pedicle screws” on either side of the spine to securely span the distance between those vertebrae to achieve fixation (restraining any movement).
Beyond this, specific patient situations influence the details: the exact approach to replacing the damaged disc, the trade-offs for surgeons to consider when choosing one disc-replacement material/design over another, and where the technology is headed in coming years.
Spinal Implant Design Evolution
For decades, traditionally manufactured implants have come in a variety of sizes and shapes for an optimal fit. At various times resembling a thick rectangle, an oval, a wedge or some combination thereof, most implants are of fixed dimensions; a few configurations can be modified once in place, with surgeons using a miniature “tire jack” device to finalize the desired side-to-side or front-to-back alignment.
More commonly, medical device manufacturers offer a range of models featuring the same outer dimensions but a variety of wedge angles (called lordotic angles – the anterior to posterior slope). Various implant configurations must be offered because different geometries work better with different surgical approaches: being inserted through the back (posterior), toward one side of the posterior (transforaminal), from the front (anterior) or directly through the side (lateral).
Lastly there’s the structure of the implant itself. It must incorporate open spaces through which new bone can grow, in order to fuse the superior and inferior vertebral bodies together. Surgeons usually insert bone-graft material (often from the patient’s own hip) directly into the gaps in the implant to encourage this osteointegration. This greatly improves the long-term strength.
Andy Christensen, the founder and former president of medical 3D printing firm Medical Modeling (now part of 3D Systems) is one of the best-known names in the field of medical 3D printing. He can tell you the past, present and a fair amount of the future surrounding 3D printed medical devices. “Before 3D printing,” he explains, some spinal cages were made of titanium that was machined or cast. Since they were difficult to machine or cast, and costly, you couldn’t get really complex with the design.”
For these and other reasons, says Christensen, over the past ten years or so there was a huge move away from titanium to the high-strength thermoplastic known as polyether ether ketone (PEEK). Not only was it easier to manufacture more complex shapes but it had the advantage of being radiolucent (i.e., it didn’t block x-rays). But a major downside with PEEK is that the bone does not attach well to it. The two surfaces could always be peeled apart from one another, so the connection was not the best.
A Return to Titanium, with Improvements
3D printing opened up a world of geometric possibilities for all medical implant designs, letting surgeons and engineers work together to create improved structures. Cranial plates, acetabular hip sockets and replacement mandibles are just a few of these end-uses; they often took advantage of printing technology that incorporated microporous (trabecular) surface textures to promote bone in-growth.
In the field of 3D printed spinal implants, the bicompatibility of titanium (Ti6Al4V) combined with 3D printing’s inherent freedom of geometry offers seemingly limitless design possibilities. The first company to make this connection and achieve FDA clearance for 3D-printed spinal implants was 4WEB Medical, in 2011, but it wasn’t just because they were good at spatial geometry. As important as it is to provide an open architecture and a large area in the implant for contiguous bone growth, the implant must also provide strength. Here’s where the company shines.
4WEB Medical holds over 20 issued and pending patents with names such as “Programmable Implants and Methods of Using Programmable Implants to Repair Bone Structure” that describe aspects of its novel implant geometry. Jessee Hunt, 4WEB president and CEO, says, “With microporous metal, bone will only grow into the surface between 1.0 and 1.5 millimeters deep. Bone will attach to it but will not grow all the way through.” Since the FDA requires a contiguous column of bone (fully connecting the two vertebrae), he notes that most 3D printing approaches have simply included creating large holes through the lattice structure of the implant.
“The goal is fusion, not just fixation,” explains Hunt. “Other (designs) get fusion but we truly take advantage of the opportunities 3D printing allows, and we get improved clinical benefits.” All 4WEB spinal implants display a very visible truss-and-strut-based, open architecture; not only does this provide light-weighting and a path for bone growth, it is highly engineered for optimal load bearing. (A detailed explanation is presented in the presentation, “THE MECHANICAL AND BIOMECHANICAL PRINCIPLES OF TRUSS STRUCTURES FOR INTERBODY FUSION”) The mechanical strain experienced by each strut transfers to adjacent cellular material, stimulating bone formation and minimizing inter-vertebral compression (subsidence).
Outer edges of the implants are machined smooth after printing for optimal insertion during surgery, but all internal surfaces are purposefully printed with a hierarchical surface roughness that ranges from macro- to nano-scales. The resulting surface area of this landscape is three times that of comparable spinal implants and can only be achieved with 3D printing.
4WEB Medical prints in titanium on Arcam EBM systems. The company recently announced it has surpassed the 30,000-implant milestone in just five years of surgical use.
A Sampling of Companies Producing 3D Printed Spinal Implants
Keep an eye on this space, as more companies join the 3D printed spinal implant marketplace; this list is undoubtedly incomplete and changing weekly. Note: some of the implants exist as an off-the-shelf product line, some are patient specific (custom-made from CAT scan and MRI data), and some are awaiting FDA approval for use in the United States.
EIT Emerging Implant Technologies
Si Bone (sacroiliac joint)
Subscribe to our FREE magazine, FREE email newsletters or both!
About the Author
Pamela Waterman worked as Digital Engineering’s contributing editor for two decades. Contact her via .(JavaScript must be enabled to view this email address).
Follow DE