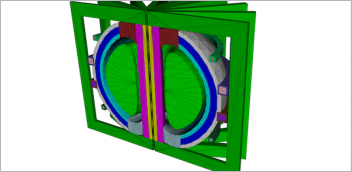
UConn Students Build 3D Printed Artificial Kidney
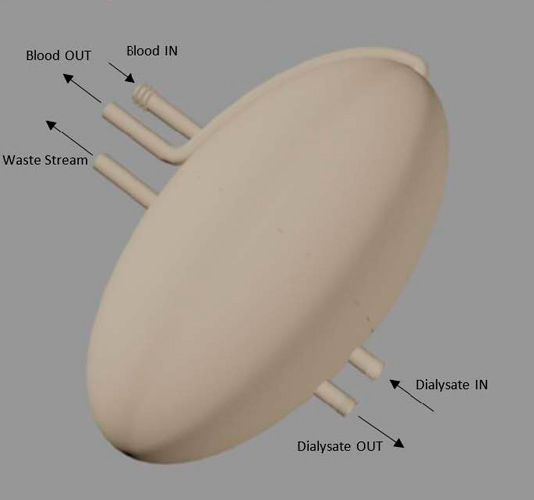
AutoCAD rendering of the artificial kidney, which was designed with all the functions of a biological kidney. Courtesy of Benjamin Coscia.
May 13, 2014
The last couple of years have seen a fair amount of progress in bioprinting new organs for needy patients. While the technology is promising, it’s still years away from becoming available for use, and, at least initially, the cost of a 3D printed organ is likely to be somewhat prohibitive. Those stumbling blocks don’t mean that additive manufacturing (AM) is useless for organ replacement surgery, just that the technology has to be applied in a different manner.
Students at the University of Connecticut (UConn) have developed an artificial kidney using AM. Rather than attempting to build the organ using bioprinting, the students used more traditional additive techniques along with AutoCAD to build a functional kidney made of artificial materials.
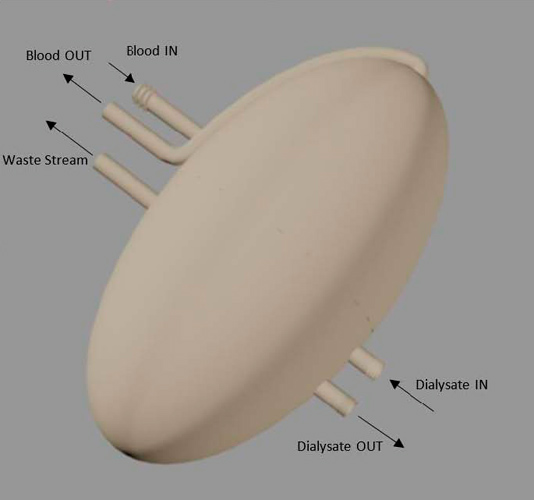 AutoCAD rendering of the artificial kidney, which was designed with all the functions of a biological kidney. Courtesy of Benjamin Coscia.
AutoCAD rendering of the artificial kidney, which was designed with all the functions of a biological kidney. Courtesy of Benjamin Coscia.Statistics available from National Kidney Foundation indicate there are around 100,000 patients awaiting kidney transplants in the US, but only 14,000 transplants take place in a given year. Worse, more patients are constantly being added to the waitlist, with around 2,500 new patients added each month. Those numbers are only likely to increase as the Baby Boomers continue to age.
A potential solution to the problem is building kidneys to fill the gap between available organs for transplant and the remaining patients that require a kidney. Led by Anson Ma, assistant professor in the Department of Chemical and Biomolecular Engineering and the Institute of Materials Science, two teams of chemical engineering students were given the job of using AM to design an artificial kidney for their Senior Design Project.
The two teams set about their project in different ways. One group focused on electrodialysis and forward osmosis, while the other decided to work with hollow fiber membrane technology commonly found in traditional hemodialysis treatments. Benjamin Coscia, a member of the second team, explained the reasoning behind their approach.
“Because 3D printing resolutions are not currently low enough to print a structure which will actually filter blood, the file is of only the shell of the kidney,” said Coscia. “Hollow fiber membranes will be installed on the inside to do the filtration function. The kidney will then be sealed together using the threads and sealing o-rings. A fluid called dialysate will be circulated on the outside of the membranes, inside of the shell, which will cause flux of components from the blood. A waste stream maintains the person’s ability to urinate. The outside of the shell can be used as a substrate for growth of biological material for ease of integration into the body.”
Projects like this not only showcase the flexibility of AM, but also highlight how the technology can be used to quickly produce prototype results. If UConn’s kidneys prove viable, they could join the list of other AM-built medical devices that have already helped save lives.
Below you’ll find a video discussing some of the medical uses of AM.
Source: Uconn
Subscribe to our FREE magazine, FREE email newsletters or both!
About the Author
John NewmanJohn Newman is a Digital Engineering contributor who focuses on 3D printing. Contact him via [email protected] and read his posts on Rapid Ready Technology.
Follow DE